Anesthesia is one of the most common practices used in wildlife medicine. As you can imagine, most wildlife is not keen to being handled by humans and some species are too dangerous to handle without anesthesia. Some of the more advanced treatments and diagnostics require the animal to be anesthetized to perform. Even X-rays can be difficult in these species when not anesthetized because they won’t stay in the position needed. In human medicine, anesthesia is often seen as a scary process. Many complications are associated with anesthesia and some people suffer adverse consequences afterwards. Luckily, our veterinary species seem to tolerate it very well. Wildlife is resilient and can handle a lot more than we give them credit for.
There are two main protocols for administering anesthesia: total intravenous anesthesia (TIVA) and inhalants. In wildlife settings, TIVA is typically used because the procedure is either done in the field or the facility does not have a gas anesthesia machine. When inhalants are used, some intravenous drugs are still given (pre-medication) to offset the side effects of inhalant anesthesia and to make recovery easier. Inhalant anesthesia with premedication is the most used anesthesia in small animal hospitals and human hospitals. Inhalant anesthesia alone can be used for short, non-painful procedures in wildlife when its available. In the teaching hospital at our university, we commonly use inhalants alone to sedate an animal for X-rays or ultrasound.
Delivery of anesthetics can be tricky as well. There are many different methods of delivering anesthesia.
- Dart
This is the most common method in wildlife because we often can’t get close enough to our patients to administer anesthesia by hand. Darts can be administered through 3 methods: dart gun, pistol, and blow dart. Dart guns allow you to be farther away, more accurate, and have more power to get through tough skin. However, they can cause muscle trauma in smaller animals or if shot from too close. Pistols are CO2 powered devices that act like a dart gun but with less force. Blow darts require very close range and are not as accurate, but they have minimal tissue trauma.

- Injection
There are two main methods of administration of anesthetics through injection: intramuscular or intravenous. In hospital or clinic situations, anesthetics would most like be given intravenous. These facilities will place intravenous catheters before an anesthetic procedure, so they have quick, easy access to a vein to administer the drugs. In wildlife and places with limited resources, we tend to opt for intramuscular injections because they are easier to administer faster. Darts are shot into large muscle bodies for the drugs to be dispersed intramuscularly. Intramuscular injections have a slower onset of effects than intravenous administration.

- Inhalation
If inhalant anesthesia is available, it is a fast and effective administration method. There are three main methods of administering inhalant anesthesia: mask, chamber, and endotracheal tube. Masks are a fast method of administration in dogs and cats. These masks come in different sizes that can be fit to the size of the animal. However, these masks typically don’t fit on animals with different shaped faces or very small animals. In these cases, chambers can be used. These are boxes that have a port for the gas anesthesia to be attached and put into the chamber. The animal will then breathe in the anesthesia until they are safe to handle or asleep enough for the procedure. We use these chambers in reptiles and small mammals. The final method is endotracheal tube. This is used in all cases where inhalants are available once the animal is anesthetized through another method. In many small animal hospitals and private practices, the preferred method is to administer the pre-medications through an intravenous catheter to sedate the animal enough to place the endotracheal tube. Once the tube is placed, gas anesthetics are run through the tube and used to maintain the plane of anesthesia throughout the procedure.

There are many different drugs that can be used for anesthesia. Each of them has side effects so to achieve safe and effective anesthesia we use a combination of these drug classes. Some of these classes would not achieve an adequate anesthetic plane on their own but have other desired side effects that make anesthesia better. By combining the drugs, we decrease the amount of side effects seem from each one by decreasing the dose used. Without going into too much pharmacology, I will go through the drug classes we use and what they are used for.
- Dissociatives: This is the drug class that includes ketamine. Ketamine provides pain relief and general anesthesia. It is one of the drugs that can be used on its own as an anesthetic. Side effects include high blood pressure, respiratory depression, increased body temperature, vomiting, and seizures in high doses. Animals anesthetized with ketamine will have muscle rigidity and their eyes will remain open. Ketamine causes a unique breathing pattern characterized by rapid breaths followed by holding their breath.
- Opioids: This is a huge class of drugs with many different effects. In the case of anesthesia, we use them mostly for their pain relief effects. Opioids also have sedative effects. Side effects include respiratory depression, nausea, and vomiting. Commonly used opioids in wildlife medicine are butorphanol, etorphine, and fentanyl.
- Benzodiazepines: Diazepam, midazolam, and zolazepam are the most used drugs in veterinary medicine for anesthesia. The main function of adding a benzodiazepine into your combination of anesthesia is for muscle relaxation. These drugs also have an anti-anxiety effect which can offset dysphoria associated with opioids and ketamine. Side effects are very minimal, but they do not have sedative effects in healthy, adult patients. We do not typically use these drugs in free-ranging wildlife because they are non-reversible, and you want the animal to be able to get up and walk away as soon as you are done.
- Alpha-2 agonists: These drugs provide heavy sedation and hypnosis in our animal patients. This class includes xylazine, medetomidine, and dexmedetomidine. Side effects include low blood pressure and decreased heart rate, occasionally vomiting, urination, and high blood sugar.
- Inhalants: The most used inhalants are isoflurane and sevoflurane. Inhalants are much easier to control because you can finetune the amount that the patient is getting at any one time. Inhalants on their own cause great muscle relaxation and sedation. Inhalant side effects include respiratory depression and hypotension.
*Note: this list is not exhaustive. There are tons of anesthetic drugs that are not included in this list that are commonly used.
In a hospital setting, opioids, benzodiazepines, and opioids would serve as your pre-medications. Ketamine or inhalants would then be used for induction of anesthesia depending on what is available. In wildlife, we administer pre-medication and induction agents at the same time because they are administered in the same way.
When using anesthesia, it is also important to have emergency drugs on hand and easy to access. Epinephrine, norepinephrine, dopamine, and dobutamine are the most common emergency drugs used in veterinary medicine. Opioids and alpha-2 agonists can also be reversed. These drugs are used if the animal begins having an adverse reaction to the anesthetic drugs or the side effect overwhelm the animal and you need them to wake up immediately.
In the US, many of these drugs are regulated by the government and require a special license to use and handle. In Malawi, they do not have regulations like these. However, drugs are not widely available in country, so they have a much smaller spectrum of drugs to choose from. For example, they have access to medetomidine but not dexmedetomidine. Drugs are also very expensive in Malawi so choices are often selected based on price and availability.
When a patient is under anesthesia, there are multiple parameters that are monitored to determine how anesthetized the patient is, how they are handling the anesthetics, and their overall health status during the anesthetic event.
- Vitals:
Temperature, heart rate, and breathing rate should be monitored throughout the entire procedure. As you can see from above, all these parameters are affected by the anesthetic drugs that we use. It is common for the breathing rate to be lower than normal, but the breaths should remain consistent and maintain depth. Increases in heart rate or breathing rate can mean that the animal is beginning to wake up or feel what is happening to them. Temperature regulation is not functional during anesthesia and low body temperature is common because of the cold surgical table and environment. If equipment is available, blood pressure and oxygen saturation are important vitals as well. Many of the anesthetic drugs have effects on the respiratory and cardiovascular system so these parameters are important to monitor as well if possible.

- Presence of reflexes:
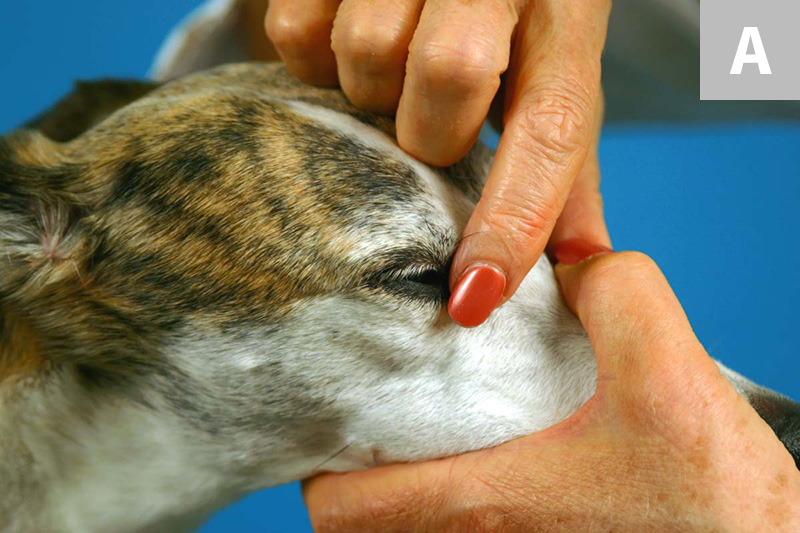
Due to the sedative effects of anesthetics, many reflexes are not functional under anesthesia. The main one that we check during a procedure is the blink reflex. This is the one most used because the head is usually not involved in the procedure, so it is easy to access and easy to see. An animal should not blink when at an adequate plane of anesthesia. If they begin blinking, it usually means that they are becoming too light and might need more anesthesia or the inhalants turned up.
- Jaw tone:
When animals are at an appropriate plane of anesthesia, they should not have any jaw tone. This means that you can easily open and close their jaw. When patients begin waking up, they will clench their jaws and you will not be able to open it.
- Eye position:
This is a very difficult one to monitor because there is huge species variation on normal eye position and where the eye sits normally. Most of the time, the eye should be down and towards the nose, exposing a large amount of the white of the eye, when they are at an adequate plane of anesthesia. If the depth of anesthesia increases to a dangerous level or the animal begins waking up, the eye will become central. Ketamine negates all of this because the eye will remain central the entire time the animal is under the effects of anesthesia.

Anesthesia is a stressful procedure for everyone involved. The patient is in a vulnerable position and the veterinary staff is responsible for monitoring many aspects at the same time. In wildlife, anesthesia allows us to provide treatment to animals that otherwise would not be safe to handle. Research has improved anesthesia immensely and many animals handle the anesthetic drugs very well. We have developed protocols that are safe, reduce the side effects and adverse events, and allow us to provide treatment.
Medical Terminology Dictionary
- Intravenous: into a vein
- Intramuscular: into a muscle
- Endotracheal tube (E-tube): a tube placed into the trachea to provide oxygen and inhalant anesthesia to a patient
- Analgesia: pain relief
- Hypertension: high blood pressure
- Hypotension: low blood pressure
- Apnea: absence of breaths
- Dyspnea: irregular breathing
- Bradypnea: low breathing rate
- Tachypnea: high breathing rate
- Hyperthermia: increased body temperature
- Hypothermia: decreased body temperature
- Emesis: vomiting
- Ataxia: muscle rigidity
- Apneustic breathing: the unique breathing pattern associated with ketamine that is characterized by rapid breaths followed by a breath hold
- Anxiolytic: anti-anxiety
- Bradycardia: decreased heart rate
- Tachycardia: increased heart rate
- Palpebral reflex: blink reflex
- Ventromedial: down and towards the center; the eye position desired during an adequate anesthetic plane

Leave a comment